In 1976, James K Styner, an orthopaedic surgeon from Lincoln, USA, crash-landed his light aircraft into a field in rural Nebraska. Styner’s family was with him in the plane. His wife died instantaneously. Three of his four children were knocked unconscious by the impact. The fourth, Chris, fractured his forearm bones. Styner himself fractured his facial bones and ribs.
Styner provided his children what little care he could at the crash site. He and Chris extricated the unconscious children, walked to the nearby road and flagged down a passing car. They got the children into the car and rushed them to a hospital in the nearest town, only to find it closed. Styner contacted the doctor and got it opened, but found to his dismay that the place was poorly equipped, and its personnel inexperienced. He was particularly horrified to see his unconscious children being moved without neck protection, a potential cause of irreparable spinal cord injury. He finally called a colleague in Lincoln who arranged for a helicopter to shift them all to a hospital there.
On returning to Lincoln, Styner could not forget the rural hospital. He said, “When I can provide better care in the field with limited resources than my children and I received at the primary facility, there is something wrong with the system and it has to be changed.”
He changed the system. Styner and his colleagues forged a system of examining and treating trauma victims which is today accepted and used all over the world. He introduced the treatment protocol in 1978. This was the prototype of ATLS as it is known today.
Advanced Trauma Life Support (ATLS) is a training programme conducted by the American College of Surgeons. It focuses on initial assessment and treatment of trauma victims. ATLS seeks to identify the early causes of death following major trauma, managing these causes as they are identified in a prioritised fashion. The causes of death following trauma are time-bound and well-defined. The most dramatically-presenting injuries are often not the ones which kill. The broken femur protruding out of a thigh may be visually alarming, but is not immediately fatal. Unnoticed bleeding into the abdominal cavity kills patients faster, and more surely.
ATLS is strikingly different from traditional methods of patient management. The usual clinical practices of taking a detailed history and lengthy examination– inspection, palpation, auscultation- followed by investigations do not work in the emergency setting. Time is crucial here. Every patient is presumed to have major life threatening injuries until they are ruled out one by one.
ATLS begins with a primary survey, the ABCDE of trauma care. At each step, the examiner takes care to protect the cervical spine.
A is for Airway. The patient with a facial trauma may choke on his own blood and die. Death arrives in seconds when the airway is blocked and the brain is deprived of oxygen. This risk is higher in victims who are unconscious. In these cases, an endotracheal tube is inserted into the trachea and artificial ventilation started.
B stands for breathing. The airway has been cleared. But is the patient breathing? If he is, is he doing it well? Does he have sufficient oxygen in his blood? If no, why not? Has broken ribs punctured his lungs? Is air leaking out of his lungs? Is the chest flooded with blood? These potentially fatal causes must be identified and dealt with early, often by inserting a tube into the chest to evacuate blood or air. These patients are also candidates for intubation and ventilation.
C is circulation. Is the heart working? Is blood pressure maintained? If the blood pressure is falling what could be the reason? Is there a bleeding external wound? Or, more seriously, is there an internal injury which is draining blood into a body cavity? Is there a chest injury, a ruptured liver in the abdomen, a torn spleen, a bleeding artery? Is the pelvic ring broken?
D is disability. What is the patient’s neurological status? What is his level of consciousness? AVPU is a mnemonic to quickly check brain function. A is an alert patient. The patient reacts normally to stimuli. V is a patient who responds to verbal stimuli. He responds but the responses are blunted. P is the patient who responds only to pain. U is unconsciousness, a sign of serious head trauma. However, unconsciousness may be from causes other than head injury. It may be due to a low oxygen level in the blood, or low blood sugars.
The Glasgow Coma Scale (GCS) is a more accurate measure of brain activity. It is a scoring system with a high score of 15. A score of 15 rules out a head injury at the time of examination. The lowest score is 3. 3 out of 15, which signifies major brain injury, a life threatening situation.
E is exposure, and the patient is stripped naked to see if there are injuries which may otherwise be missed, bleeding from external genitalia, or from the anal orifice.
An experienced emergency doctor at work is a fascinating sight. Responses are at a subconscious level, automatic, similar to that of a well-set batsman at the crease. There is little time for thought: The patient is unconscious, check airway, there is bleeding, suction. He is breathing now, oxygen saturation is fine, that leg wound is bleeding, pressure bandage. What’s the GCS? And so it goes on.
The primary survey over, ABCDE assessed and managed, the neck protected throughout, the ER physician proceeds to the secondary survey.
This is a war zone. Trauma care is meditation in the middle of a madding crowd. One must deal with more than one critically-ill patient at a time, their frightened and angry relatives, and noisy drunks who are always present. In many of our hospitals, doctors and nurses must manage not just the patient but also these anxious and unruly crowds. This may require considerable patience and skill.
Doctors fresh out of medical college often do not have the required skill or maturity to control these situations. But do it they must. Specialist doctors less often encounter the front line. They are able to work in relatively quieter zones within operation theaters and ICUs.
The emergency physician’s role is thus well defined. They are specialists who deal with emergency care. In some of our bigger hospitals, these doctors now direct emergency care. They are the primary attenders of not only accident victims but also all other forms of medical emergencies, ranging from burns to heart attacks to animal bites.
In the hospital where I work, three emergency physicians manage the Casualty Department. A team of casualty doctors and nurses whom they have trained assists them. This hospital is by the national highway and receives accident victims, all day long, and all night.
Most of these injuries are from high-speed impacts, the price we pay for life in the fast lane. These are polytrauma victims, where more than one body system is injured. The causes of death for these patients are numerous, and well defined. Patients may need multiple surgeries. Treatment requires exact planning and timing of surgeries is crucial. Not all hospitals have the necessary infrastructure to treat these patients. A team of specialists are needed and a lot of expensive equipment. Importantly, the critical care specialist plays a vital role in coordinating the entire treatment.
But primary care is still the ATLS and the ABCDE mantra–airway, breathing, circulation disability and exposure. Stabilize first, then call in the specialists. My role as an orthopaedic surgeon begins now, with the patient stabilized, IV lines placed, the neck immobilized and fractures splinted. We now need to decide definitive care for these fractures.
Many trauma patients who arrive at our hospital are travellers from faraway places. Most are alone. Some are unconscious. We do not know who they are or where they come from. They are often brought in by the public or sometimes by the police, who leave immediately after they handover the patient. These patients’ lives now are in the hands of our trauma team.
The team treats them all. They seek out their relatives. Once the relatives arrive further treatment can be decided. But some patients cannot wait. They need immediate surgery or critical care. The patient with torn blood vessels will not wait for his or her relatives to appear, or the one with a flail chest. We must treat these patients or must refer them, most often to the Medical College Hospital.
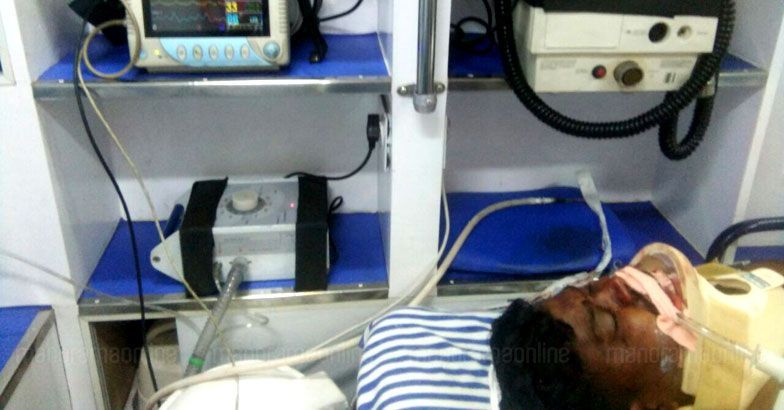
Murugan and Muthu were two such patients who we received at about 10 pm on August 6. They were brought in by the public who left soon afterwards. Muthu had a few contusions and a fractured hand, nothing serious. Murugan’s case was different. He was unconscious, with a GCS of 3/15. He had a fractured elbow, and a degloving injury of the knee. Murugan was critically ill.
The team tried to stabilize him. He was intubated and ventilated. IV cannulas and splints were placed. He needed a neurosurgeon now, CT scans, intensive care, and perhaps an emergency surgery to relieve compression within the brain. Our neurosurgeon was unavailable that day and hence Murugan was referred for expert care to Thiruvananthapuram Medical College in an ambulance with ventilator facilities. The ambulance driver contacted an NGO and transferred him to a nearby private hospital.
What happened next is now the stuff of heated discussion in the media. Murugan was taken to seven other hospitals, we are told, all of which denied him treatment. Murugan’s case is primetime TV today. Youth organisations protest, the Health Minister cries negligence, the Chief Minister apologises on the floor of the Assembly and the social media heaps abuse on doctors and hospitals. And the State Human Rights Commission has ordered an inquiry.
An inquiry commission has been instituted. This is indeed needed. There must be an exhaustive inquiry. If Murugan was denied treatment those responsible must be punished.
We must, however, realise that this is not a first-time event. Even as you read, an accident victim lies on a hospital trolley somewhere in Kerala. No one knows who he is. He needs expert care at a high-level centre. What must be done? Do we place him in an ambulance and carry him around from hospital to hospital and ask for a ventilator, a neurosurgeon? That is what we do now, what we have been doing for years now. We see a hundred Murugans in our hospitals every month, a hundred potential deaths, a hundred cases each day who need reference for expert care.
This is a hidden human rights violation, the elephant sitting in the emergency room which no one wants to talk about. Every year about 5,000 people die on our roads from road traffic accidents. Ten people leave their homes every day, and never return. We are fast approaching the time when we can claim an accident victim in each home, a road kill in each family.
Most trauma victims are alone when they reach hospital. This is not about Murugan. This is about you or me and when we lie alone on hospital trolleys gasping for air, semiconscious, blood filling our chests, livers ruptured, bones crushed, and the doctor says, “I’m sorry but we need to shift this patient now,” what next? Where will we be shifted? Will we be taken on our last tour connected to a ventilator in an ambulance, siren blaring, beacons flickering, a guided tour of hospitals until our brains switch off and our hearts stop?
There are no guidelines for these cases and no one is talking about this. Meanwhile heated discussions will continue, until Murugan is forgotten and the next actor’s sex life becomes the latest show in town.
What can be done? There are many things that can be done before the victims reaches the hospital, like improving ambulance services and giving life support training to emergency technicians in ambulances. But we can discuss these later. We will now talk about hospital care and how it can be improved.
We must ensure good primary care in our emergency departments. Doctors trained in emergency medicine save lives and centres which routinely receive trauma patients should be manned by them. ATLS training should be given in medical colleges. Certification and periodic renewal should be mandatory for all casualty doctors. This single step will ensure a qualitative improvement of care even in our smallest hospitals.
A central control room with a database of emergency facilities is the need of the hour. Consider a patient with a vascular injury to his leg. Once the patient is stabilized the doctor can call up the central control room and ask for a vascular surgeon. The control room can look up the nearest available centre with this facility, confirm availability and arrange transfer. In Murugan’s case, the control room would have looked for a hospital with neurosurgical and critical care services. Transfers would have been arranged seamlessly and by the time Murugan reached the receiving hospital CT scan and OT facilities would have been arranged and waiting.
Such a control room in this day and age is not a difficult thing to set up given the political will. The police, private hospitals and organisations like the IMA can contribute.
A citizen’s life is the State’s responsibility. Most accident victims are young and productive. They often have no other medical conditions. These 5,000 annual deaths and an equal or greater number of disabled victims translate to a huge loss for the State. The State must fashion proper guidelines.
Murugan’s death, like Styners’s loss, should not be forgotten. His death must be taken as a landmark, a point where we decide to take responsibility to change the system. This is a system failure, and if we are satisfied merely by seeking out scapegoats to punish, and forget the larger picture, we will have many more Murugans on our hands. The system must change.
Meanwhile injuries are better prevented than cured. About once a week or so a patient walks into my clinic with minor injuries. “I had my helmet on,” he says, “so nothing happened when my head hit the post.” I hear this all the time.
Keep your eyes on the road at all times when driving. Wear seat belts. Do not drive with children on the front seat. Walk on the right side of the road. Use Zebra crossings.
Drive carefully. Slow down.
The Emergency Department is the place you are brought when you become helpless. One moment you are in the full confidence of health, and the next you lie on a trolley unable to move without help. I once saw a grown man lying on a trolley with a broken femur sobbing like a child. His daughter, a little girl, was in the next cubicle with multiple fractures and wounds. She was screaming in pain and fear. He was crying more from helplessness than from his fracture.
Please do not come to our emergency departments to see us. They are not nice places to visit.
Dr. Viswanathan K. is an orthopaedic surgeon who practices in a private hospital in Trivandrum. You can read all columns by Dr. Viswanathan here.
This article was initially published in Malayalam on the Facebook page ‘Info Clinic’, a simple initiative by a group doctors who work together to improve public health of Kerala. The article was translated and re-published following a special arrangement with Info Clinic.
Cover image courtesy: Manorama Online